Introduction
Running a mental health practice in the USA today isn’t just about providing quality care—it’s also about navigating an increasingly complex billing landscape. From insurance verification to claim submission and compliance requirements, administrative burdens can quietly eat into your time and revenue.
That’s where a reliable mental health billing and coding company becomes more than just a support system—it becomes a strategic partner. Whether you’re a solo therapist or managing a multi-provider clinic, having experts handle your billing processes can significantly improve cash flow, reduce denials, and allow you to focus on what matters most: patient care.
In this article, we’ll explore how mental health billing works, why outsourcing is gaining traction, and how to choose the best partner for your practice.
Understanding Mental Health Billing: More Than Just Claims
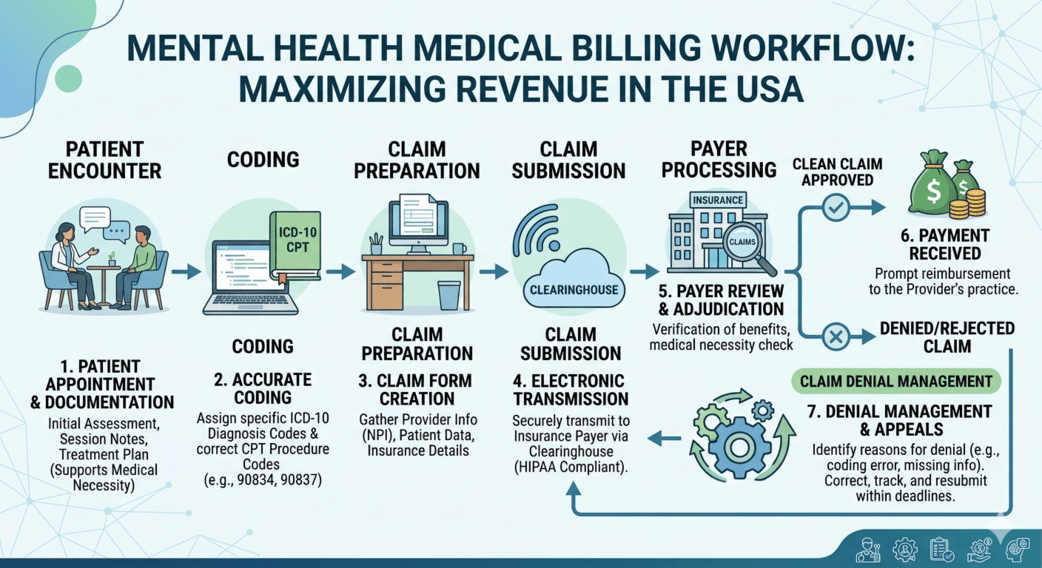
Mental health billing is different from general healthcare billing. It involves unique coding structures, session-based services, and varying insurance policies.
A mental health billing specialist must understand:
- CPT codes for therapy sessions (e.g., 90834, 90837)
- Time-based billing structures
- Telehealth billing regulations
- Insurance-specific authorization rules
- Documentation compliance
Even a small coding error can lead to claim denials or delayed payments. That’s why many providers turn to mental health insurance billing services for accuracy and efficiency.
Why Mental Health Providers Are Outsourcing Billing
The demand to outsource mental health billing services has grown rapidly in recent years—and for good reason.
1. Reduced Administrative Burden
Handling billing in-house requires hiring, training, and managing staff. Outsourcing eliminates this overhead while improving efficiency.
2. Improved Revenue Cycle
A professional mental health medical billing solution ensures:
- Faster claim submissions
- Reduced denials
- Quicker reimbursements
3. Access to Experts
A mental health billing consultant brings deep knowledge of payer rules, coding updates, and compliance requirements.
4. Scalability
As your practice grows, outsourced billing adapts without the need for additional internal resources.
Key Services Offered by a Mental Health Billing Agency
A reputable mental health billing agency offers end-to-end solutions tailored to therapists, psychologists, psychiatrists, and counseling centers.
Core Services Include:
- Insurance eligibility verification
- Prior authorization management
- Accurate coding and charge entry
- Claims submission and tracking
- Denial management and appeals
- Payment posting and reporting
Many mental health billing companies also provide customized dashboards, giving you real-time visibility into your revenue.
What Makes the Best Mental Health Billing Agency?
Not all billing partners deliver the same results. Choosing the best mental health billing agency requires careful evaluation.
Look for These Qualities:
Industry Expertise
A professional mental health billing company should specialize in behavioral health—not general billing.
Compliance Knowledge
They must stay updated with HIPAA regulations and payer-specific policies.
Transparent Reporting
The best agencies provide clear performance metrics and regular reports.
Dedicated Support
A reliable mental health billing provider offers personalized account management.
Technology Integration
Seamless integration with EHR systems is essential for efficiency.
Real-World Example: How Outsourcing Improves Revenue
Consider a mid-sized therapy clinic struggling with claim denials and delayed payments. Their in-house team lacked expertise in mental health coding, leading to frequent errors.
After partnering with a top outsource mental health billing company, they experienced:
- 30% reduction in claim denials
- 25% faster reimbursement cycles
- Improved patient billing transparency
This shift allowed clinicians to focus more on care rather than paperwork.
Specialized Billing Services for Mental Health Therapists
Therapists face unique billing challenges due to session-based services and varying insurance coverage.
Tailored Support Includes:
- Accurate time-based CPT coding
- Teletherapy billing compliance
- Coordination with multiple insurers
- Patient billing and statements
Billing services for mental health therapists ensure that every session is properly documented and reimbursed.
The Role of Mental Health Insurance Billing
Navigating mental health insurance billing can be overwhelming due to:
- Pre-authorization requirements
- Coverage limitations
- Frequent policy changes
A dedicated mental health insurance billing services provider ensures that claims meet payer requirements, reducing delays and denials.
Outsourced vs In-House Billing: A Quick Comparison
| Factor | In-House Billing | Outsourced Mental Health Billing |
|---|---|---|
| Cost | High (staff, training) | Predictable & scalable |
| Accuracy | Depends on staff skill | High with specialists |
| Compliance | Risk of errors | Managed by experts |
| Efficiency | Limited | Streamlined processes |
For most practices, outsourced mental health billing offers better long-term value.
Beyond Billing: Comprehensive Support Services
A leading mental health medical billing services outsourcing partner doesn’t just handle claims—they support your entire financial workflow.
Additional Services Often Include:
- Medical billing services for complete claim lifecycle management
- Medical coding services to ensure accurate CPT and ICD coding
- Medical billing and coding services integration for seamless workflows
- Revenue cycle management services to optimize financial performance
- Credentialing services to enroll providers with insurance networks
These services work together to create a stable and efficient revenue system.
Choosing the Right Partner for Your Practice
Selecting the best outsource mental health billing and coding company requires more than just comparing prices.
Ask These Questions:
- Do they specialize in mental health billing?
- What is their denial rate?
- How do they handle compliance updates?
- Do they offer customized reporting?
- Can they scale with your practice?
A strong partnership can significantly impact your financial health and operational efficiency.
Common Mistakes to Avoid
When selecting a mental health billing services agency, avoid:
- Choosing based solely on cost
- Ignoring industry specialization
- Overlooking reporting capabilities
- Not checking client references
Cutting corners in billing often leads to larger financial losses down the line.
The Future of Mental Health Billing in the USA
With the rise of telehealth and increasing mental health awareness, billing processes are evolving.
Trends shaping the future include:
- AI-assisted coding tools
- Automated claim tracking systems
- Enhanced compliance monitoring
- Integrated EHR and billing platforms
Partnering with a forward-thinking mental health billing provider ensures your practice stays ahead of these changes.
Conclusion
Managing billing in a mental health practice is no longer just an administrative task—it’s a critical component of financial success. Working with a trusted mental health billing and coding company allows providers to reduce stress, improve revenue, and focus on delivering quality care.
Companies like 247 medical billing services understand the unique challenges of behavioral health practices and offer tailored solutions that go beyond basic billing. By combining expertise in medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services, they help practices build a strong financial foundation without disrupting patient care.
FAQs
1. What does a mental health billing and coding company do?
A mental health billing and coding company handles insurance claims, coding, payment processing, and denial management specifically for behavioral health providers.
2. Why should I outsource mental health billing services?
Outsourcing improves accuracy, reduces administrative workload, speeds up reimbursements, and ensures compliance with insurance regulations.
3. How do mental health billing specialists reduce claim denials?
They use accurate coding, verify insurance eligibility, follow payer guidelines, and proactively address errors before claim submission.
4. What services are included in mental health medical billing services?
These include eligibility checks, coding, claim submission, denial management, payment posting, and reporting.
5. Is outsourcing billing cost-effective for small practices?
Yes, it eliminates staffing costs and improves revenue efficiency, making it a cost-effective solution even for small practices.
6. How do I choose the best mental health billing agency?
Look for industry expertise, transparent reporting, strong client reviews, compliance knowledge, and scalable solutions.