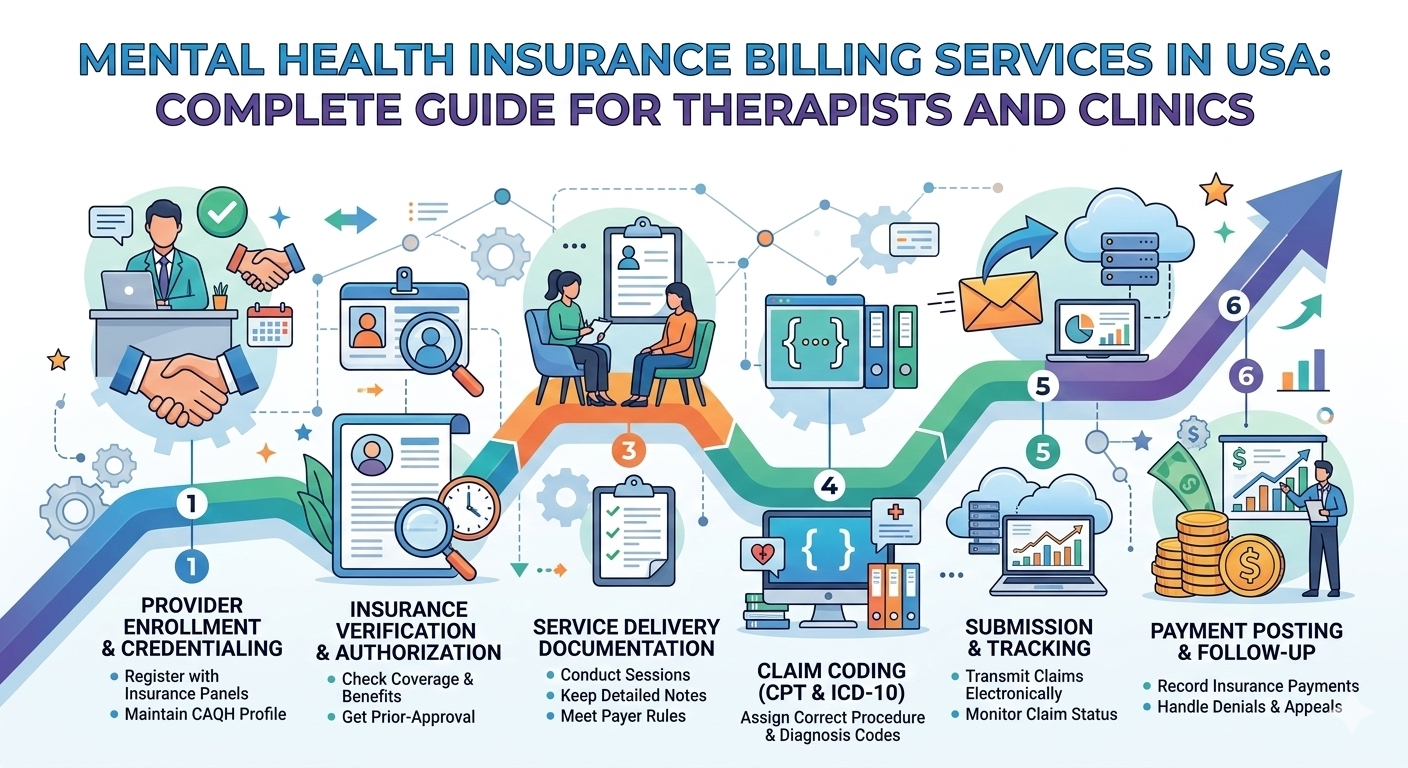
Mental health practices across the United States are experiencing a significant increase in demand for therapy, counseling, and psychiatric care. While this growth is positive for patient care, it also creates administrative pressure for providers managing complex billing processes. Mental health insurance billing involves multiple coding standards, payer rules, and documentation requirements that differ from general medical billing.
Because of these complexities, many practices rely on a specialized partner. Choosing the best mental health billing agency can make the difference between stable revenue and frequent claim denials.
A professional billing partner helps practices manage claims, verify insurance coverage, reduce errors, and maintain consistent cash flow. This article explores how mental health billing works, why outsourcing is becoming common, and how providers can identify the best mental health billing services for their practice.
Why Mental Health Billing Is More Complex Than General Medical Billing
Mental health providers face unique challenges when submitting claims to insurance companies. Unlike other medical specialties, behavioral health billing often includes longer treatment plans, recurring therapy sessions, and strict documentation rules.
Several factors contribute to this complexity.
-
Insurance policies often require prior authorization for therapy sessions
-
Payers have strict guidelines for psychotherapy CPT codes
-
Documentation must match treatment plans and progress notes
-
Telehealth rules vary between states and insurers
-
Denials occur frequently due to coding or eligibility issues
Because of these factors, many clinics depend on a mental health billing specialist who understands payer rules specific to psychotherapy, counseling, and psychiatric services.
A reliable mental health medical billing solution ensures that providers can focus on patient care while billing experts manage the financial side of the practice.
What a Mental Health Billing Agency Actually Does
A professional mental health billing agency manages the complete billing cycle for behavioral health practices. This process includes everything from patient eligibility verification to final payment posting.
Most mental health billing services agency providers offer the following functions:
-
Insurance eligibility verification
-
CPT and ICD coding for behavioral health services
-
Claim submission and electronic billing
-
Denial management and resubmission
-
Payment posting and reconciliation
-
Revenue cycle reporting and analytics
A mental health billing and coding company also keeps track of insurance updates and payer policies to prevent compliance issues.
When handled correctly, mental health medical billing services improve claim acceptance rates and shorten reimbursement timelines.
Key Benefits of Outsourcing Mental Health Billing
Many therapy clinics and psychiatric practices now choose to outsource mental health billing services instead of managing billing internally. Outsourcing allows providers to work with experienced professionals who specialize in behavioral health claims.
Some of the most important benefits include:
Higher Claim Approval Rates
Experienced mental health billing specialist companies understand payer requirements and coding standards, which reduces claim rejections.
Lower Administrative Burden
When practices adopt outsourced mental health billing, staff members can focus more on patient care and less on paperwork.
Faster Reimbursements
A professional mental health billing provider submits clean claims quickly and follows up with insurance companies to accelerate payments.
Reduced Compliance Risk
A mental health billing consultant helps practices stay compliant with HIPAA regulations and insurance guidelines.
Scalability for Growing Practices
As practices expand, a mental health billing services company can easily handle higher claim volumes without requiring additional internal staff.
For many providers, mental health medical billing services outsourcing becomes a long-term strategy to stabilize revenue.
Who Needs Billing Services for Mental Health Providers
Not every healthcare organization faces the same billing challenges, but many mental health professionals benefit from specialized billing services.
The following providers commonly use billing services for mental health therapists and clinics:
-
Psychiatrists
-
Psychologists
-
Licensed therapists
-
Behavioral health clinics
-
Substance use treatment centers
-
Telehealth counseling platforms
-
Community mental health organizations
These professionals often work with billing companies for mental health to ensure accurate coding and efficient reimbursement.
A professional mental health billing company understands psychotherapy CPT codes, psychiatric evaluations, medication management billing, and group therapy claims.
How to Choose the Best Mental Health Billing Agency
Selecting the best mental health billing agency requires careful evaluation. Providers should look beyond pricing and focus on expertise, technology, and industry experience.
Several factors help determine whether a company is the right partner.
Specialization in Behavioral Health
The best mental health billing company should focus specifically on behavioral health and psychotherapy billing.
Experienced Billing Specialists
A team of trained mental health billing specialist professionals ensures that coding and claim submission are handled accurately.
Transparent Reporting
A top mental health billing company provides clear performance reports showing claim status, collections, and denial trends.
Technology Integration
Modern mental health medical billing solution platforms integrate with electronic health records to streamline claim submission.
Strong Denial Management
The best outsource mental health billing and coding company actively tracks denied claims and resolves them quickly.
Practices should also ask potential partners about payer relationships, turnaround time, and compliance processes.
The Role of Coding in Behavioral Health Billing
Accurate coding is a crucial part of mental health insurance billing. Even minor mistakes can lead to denied claims or delayed reimbursements.
A qualified mental health billing specialist understands the correct use of psychotherapy CPT codes, evaluation and management codes, and diagnostic coding standards.
Common coding services provided by a mental health billing agency include:
-
Psychotherapy session coding
-
Psychiatric diagnostic evaluation coding
-
Medication management billing
-
Teletherapy coding compliance
-
Group therapy claim documentation
Professional behavioral & mental health billing services ensure that codes match documentation and payer policies.
Common Challenges Mental Health Providers Face With Billing
Without the right support, many providers struggle with billing operations. These challenges often lead practices to seek outsourced mental health billing support.
Some of the most common issues include:
-
High claim denial rates
-
Insurance verification delays
-
Confusing payer requirements
-
Missing documentation
-
Inconsistent payment follow-ups
A professional mental health billing provider helps practices overcome these obstacles by implementing structured billing workflows.
When providers partner with a top outsource mental health billing company, they gain access to experts who manage these issues daily.
Why Mental Health Billing Outsourcing Is Growing in the USA
The demand for outsourcing mental health billing and coding continues to rise across the United States. Several factors contribute to this trend.
Healthcare providers are focusing more on patient care while administrative tasks become increasingly complex. Insurance companies frequently update policies, and maintaining in-house billing expertise requires constant training.
By working with professional mental health billing companies, practices gain access to experienced teams without the cost of hiring full-time billing staff.
Many clinics also rely on mental health medical billing services outsourcing to manage telehealth claims, which have expanded significantly in recent years.
Outsourcing helps practices maintain efficiency, reduce billing errors, and improve financial performance.
Technology and Automation in Modern Mental Health Billing
Advanced billing technology plays a key role in modern mental health billing services. Today’s best mental health billing services company uses automation and analytics to streamline the entire billing cycle.
Technology-driven billing solutions typically include:
-
Automated eligibility verification
-
Electronic claim submission
-
Real-time denial tracking
-
Revenue cycle analytics
-
Secure patient data management
A modern mental health medical billing solution improves claim accuracy and ensures compliance with healthcare regulations.
This level of automation is difficult for smaller practices to maintain internally, which is another reason many providers choose outsourced mental health billing.
Choosing a Trusted Partner for Long-Term Growth
Selecting the best mental health billing services is not only about reducing administrative work. It also plays a crucial role in financial stability and long-term growth for mental health practices.
A professional mental health billing consultant can analyze billing performance, identify revenue gaps, and recommend improvements to optimize collections.
The right mental health billing services agency becomes an extension of the provider’s practice, supporting both financial operations and compliance management.
Organizations such as 247 Medical Billing Services support healthcare providers with comprehensive solutions including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These integrated solutions help mental health practices streamline administrative tasks while maintaining efficient billing processes.
Conclusion
Mental health providers play a vital role in supporting patient well-being, but the complexity of insurance billing can create significant challenges. Working with the best mental health billing agency allows practices to improve claim accuracy, accelerate reimbursements, and reduce administrative stress.
Whether a provider operates a small therapy clinic or a large behavioral health organization, partnering with a professional mental health billing company can significantly strengthen financial operations.
As insurance requirements continue to evolve, outsourcing to experienced mental health billing specialist companies ensures that practices remain compliant, efficient, and focused on delivering quality care to their patients.
Frequently Asked Questions
What is a mental health billing agency?
A mental health billing agency is a specialized company that manages insurance claims, coding, and payment processing for therapists, psychiatrists, and behavioral health clinics.
Why should providers outsource mental health billing services?
Providers often outsource mental health billing services to reduce administrative workload, improve claim accuracy, and ensure faster reimbursement from insurance companies.
What services are included in mental health medical billing services?
Mental health medical billing services typically include insurance verification, coding, claim submission, denial management, payment posting, and revenue cycle reporting.
How does a mental health billing specialist help reduce claim denials?
A mental health billing specialist ensures that claims follow correct coding standards, documentation requirements, and payer guidelines, which reduces rejection rates.
What should providers look for in the best mental health billing company?
Providers should evaluate experience in behavioral health billing, technology integration, reporting transparency, denial management processes, and compliance expertise.
Is outsourcing mental health billing and coding cost effective?
Yes. Outsourcing mental health billing and coding often reduces staffing costs, increases claim approval rates, and improves overall revenue cycle efficiency for healthcare practices.